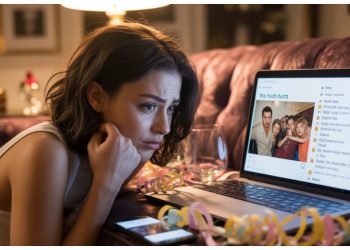
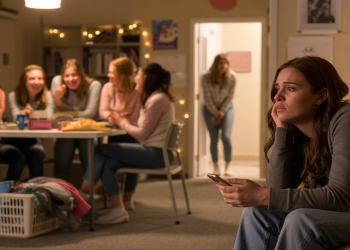Grief does not follow a deadline, even when adults remarry.
One 16-year-old Redditor shared a deeply layered story about losing his mom, going through family therapy before his dad remarried, and setting clear emotional boundaries so the new blended household could actually function without constant conflict.
And honestly? It worked.
He and his sister respected their stepmom, accepted her kids as step-siblings, and agreed on a system that allowed them to keep their late mom’s memory alive while still living peacefully in the new family structure.
But years later, the adults want a rewrite.
Now the dad and stepmom are back in therapy, not because things are exploding, but because the stepmom says she wants to be seen as a full parent instead of an “aunt figure.” The teen, meanwhile, says the original rules were agreed upon in therapy and he does not want to change them.
Cue emotional tension, pressure, and the uncomfortable question: Are boundaries still valid if they stop making the adults feel good?
Now, read the full story:



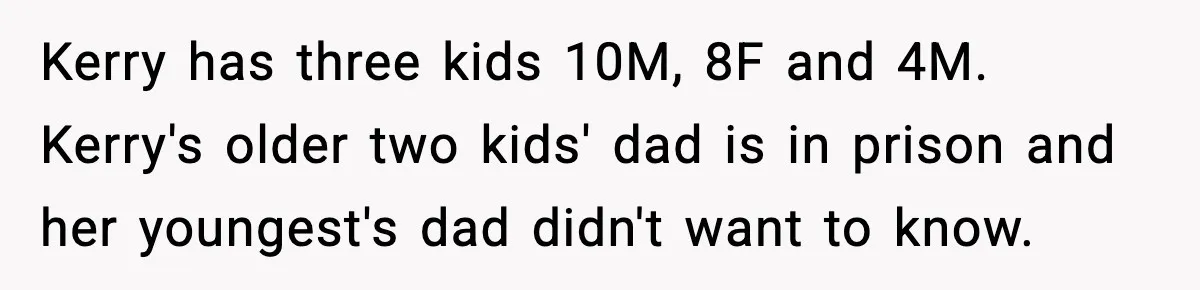























This is one of those posts where you can almost feel the quiet emotional fatigue behind every sentence. No screaming. No rebellion. No chaos.
Just a kid who went through trauma, did therapy properly, followed the agreed system, and is now being told the system should be emotionally upgraded because the adults feel ready.
That is… a very heavy ask.
Let’s start with the most important psychological truth in this entire situation.
You cannot assign a parental bond.
Family therapists consistently emphasize that step-parent relationships must be built organically, not demanded. According to the American Academy of Child & Adolescent Psychiatry, children in blended families often need time to adjust and “relationships with stepparents should develop slowly and naturally rather than being forced into a parental role.”
That aligns almost perfectly with what happened here. Therapy created a structure that reduced conflict and respected grief. That is not failure. That is successful adjustment.
Another key layer is unresolved grief.
Research in child bereavement shows that losing a parent in childhood can permanently shape attachment patterns. The Child Mind Institute notes that grieving children often hold strong loyalty bonds to the deceased parent and may feel emotionally threatened when a new adult is positioned as a replacement.
And here’s the critical nuance.
The teen is not rejecting Kerry as a person. He is rejecting the parental title.
That is a massive psychological difference.
From a family systems perspective, the boundary he set is actually quite structured and healthy:
-
Respect the step-parent
-
Keep space for the deceased parent
-
Maintain individual time with surviving parent
-
Use accurate relational labels (step vs sibling/parent)
These are not hostile rules. These are grief-informed coping mechanisms.
Now, let’s talk about therapy ethics.
When boundaries are established in therapy and agreed upon by all parties, abruptly trying to renegotiate them later can feel destabilizing, especially for teens. The American Psychological Association highlights that adolescents require consistency and autonomy in identity formation, including how they define family roles.
If a teen feels pressured to redefine a parental role before they are emotionally ready, the likely outcomes are:
-
Increased withdrawal
-
Resentment toward the step-parent
-
Breakdown of trust in therapy
-
Emotional shutdown instead of bonding
Ironically, pushing for a “closer” label often creates more distance.
There is also a subtle emotional dynamic many adults miss.
Kerry saying “I’ve come to love you and want to be a parent” is emotionally understandable. But love from an adult does not automatically create parental attachment in a grieving child. Attachment forms through safety, time, and choice, not emotional requests.
Another interesting angle raised by commenters is role imbalance. If Kerry is doing parental tasks but not receiving emotional recognition as a parent, she may feel rejected. That is a real emotional experience. However, therapy frameworks stress that step-parents should initially function as supportive adults, not replacements.
The Gottman Institute and other family researchers often recommend a “mentor or ally” role for step-parents in early years rather than immediate parental authority. This reduces loyalty conflicts in children who lost a biological parent.
And here’s the emotional core of the conflict.
The dad says, “We don’t feel like a traditional family.” But the teen is essentially saying, “That’s because we are not one.”
And that statement is psychologically accurate.
Blended families are structurally different. Expecting them to emotionally mirror nuclear families often creates pressure that therapy originally tried to reduce.
Finally, the timing matters a lot.
The boundary was:
-
Discussed in therapy
-
Agreed to before marriage
-
Maintained successfully for years
Changing it now does not feel like growth to the teen. It feels like the original agreement had an expiration date that only the adults knew about. That can damage therapeutic trust more than the boundary itself.
Check out how the community responded:
Bold summary: Many Redditors strongly defended the teen’s boundaries, emphasizing that the adults agreed to them before marriage and cannot retroactively rewrite the emotional contract.



Bold summary: Some users pointed out a worrying pattern, saying therapy now sounds less like support and more like pressure to force emotional compliance.



Bold summary: A few commenters added nuance, suggesting the stepmom may feel emotionally stuck doing parenting work without receiving a parental bond, which could be worth discussing in therapy rather than forcing labels.


This situation is not about disrespect. It is about emotional consent.
The teen did not reject Kerry as a person. He respected her, coexisted peacefully, and followed therapy agreements that were designed specifically to protect grief, identity, and stability after losing a parent.
Now the adults want a deeper emotional role, which is understandable from their perspective. Love naturally makes people want recognition and closeness.
But forced emotional titles rarely create real connection. They usually create quiet resistance.
The uncomfortable truth is that therapy did work.
It reduced conflict.
It preserved grief space.
It allowed a blended household to function.
Trying to rewrite that system because it does not “feel traditional” risks undoing the very stability therapy created.
So what do you think? Should therapy boundaries be permanent when they protect a grieving child, or is it reasonable for parents to revisit them as relationships evolve? And more importantly, can a parental bond ever be genuine if it starts with pressure instead of choice?