A hospital delay turned into one of those stories that makes you mutter, “Well, they asked for that.”
The Redditor at the center of this saga had already spent years dealing with a bad shoulder, then months dealing with a waiting list that somehow swallowed his case whole. He had the scans, the history, and the pain. What he did not have was a straight answer.
Enter his wife, a woman clearly powered by love, patience, and the kind of determination that kicks in when bureaucracy starts acting cute.
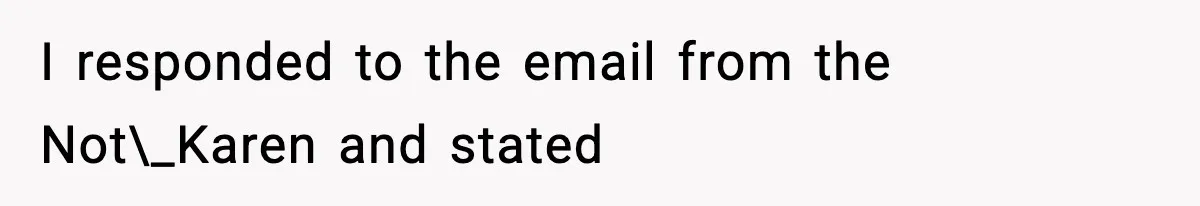
She called the hospital just to ask one simple thing. Was her husband still on the waiting list? Instead of getting help, she got stonewalled by an employee who kept repeating that the contact email was “on the website,” while refusing to say where.
That tiny detail lit the fuse.
The husband got home, opened his laptop, found not one hospital email address but hundreds, and decided to follow those instructions very, very literally.
Now, read the full story:


























































































































 Reading this, I mostly felt exhausted on the couple’s behalf.
Reading this, I mostly felt exhausted on the couple’s behalf.
Not just because of the shoulder injury, but because anyone who has ever dealt with a giant institution knows this exact flavor of frustration. You do the forms. You make the calls. You wait politely. Then one day you realize the system quietly dropped the ball and expected you to just live there.
The wife is the emotional center of this story for me.
She tried to help, kept her cool, and got rewarded with that robotic “it’s on the website” nonsense. That kind of treatment can make people feel tiny very quickly. So the husband’s response lands with a weird kind of sweetness. Petty, yes. But also deeply protective.
And that protective instinct matters in healthcare, because patient advocacy often becomes the difference between sitting in limbo and finally getting movement.
This story hooked so many readers because it speaks to a real healthcare tension. Patients are told to be patient, trust the process, and wait their turn. That works fine until communication breaks down.
Then waiting stops feeling neutral.
It starts feeling like abandonment.
The hospital employee in this story may have had legitimate privacy rules to follow. That part matters. A spouse does not automatically get access to private medical information. Even so, privacy rules do not excuse useless communication.
Healthcare systems still need to tell people how to reach the right office, what the next step is, and how to authorize someone properly. That is the part that appears to have collapsed here.
Australian guidance backs that up. The Australian Commission on Safety and Quality in Health Care says services should “support the workforce to communicate effectively with patients and their carers” and ensure “open, clear and effective communication.”
NHS England says something similar for patients waiting on planned care. Its guidance states, “Your communications should give clear, easy to understand steps for the patient’s care,” including honest timescales and what happens next.
That sentence gets right to the heart of this Reddit post.
The problem was not only the delay. The bigger problem was uncertainty layered on top of delay. Once a patient no longer knows whether they are still on a list, who can speak for them, or how to contact the right person, stress multiplies fast.
That stress is not rare in systems with long queues.
In Australia, the Australian Institute of Health and Welfare reports that in 2024 to 2025, half of public-hospital elective surgery patients were admitted within 45 days, while 6.0% waited longer than 365 days.
Those are national numbers, not a verdict on this man’s exact hospital. Still, they show why communication matters so much. When a waiting list stretches for months, patients need reliable updates or the whole process starts to feel arbitrary.
There is also a second theme here, and it is bigger than “Karen bad.”
It is advocacy.
The National Cancer Institute defines a patient advocate as someone who helps guide a patient through the healthcare system and helps them communicate with providers so they get the information they need.
That is basically what the wife was trying to do.
She was not demanding surgery in the next ten minutes. She was trying to confirm status, remove confusion, and keep the case alive. Johns Hopkins frames patient- and family-centered care around respect, coordination of care, information, communication, education, and the involvement of family and friends.
That matters because family members often act as the practical memory bank of healthcare. They chase forms, remember dates, take notes, and follow up when the patient is at work, overwhelmed, or just burned out.
So what can people actually learn from this?
First, document everything. Keep scan dates, call dates, names, departments, and promised follow-ups in one place.
Second, make authorization explicit and current. Ask the provider exactly how to record that a spouse or family member can speak on your behalf.
Third, escalate with precision. Start polite. Stay factual. Name the barrier clearly. Explain the impact. Copying half the institution should not be step one, but sometimes a paper trail needs witnesses.
Finally, separate privacy from obstruction. A staff member can refuse to disclose protected information and still give helpful process guidance. Those are not the same thing.
The satisfying part of this story is the speed of the turnaround.
The more sobering part is why it took a digital alarm bell to get there.
At its core, this post is a reminder that good healthcare communication is not a bonus feature. It is part of the care.
Check out how the community responded:
A big chunk of Reddit basically stood up, slow-clapped, and enjoyed the show. Several commenters loved the customer-service lesson and especially enjoyed imagining Karen getting called into a very awkward follow-up chat.


![Man Emails 300 Hospital Staff After Employee Refuses to Share the Right Address [Reddit User] - cackles evilly Well done!](https://dailyhighlight.com/wp-content/uploads/2026/03/wp-editor-1773048656411-3.webp)
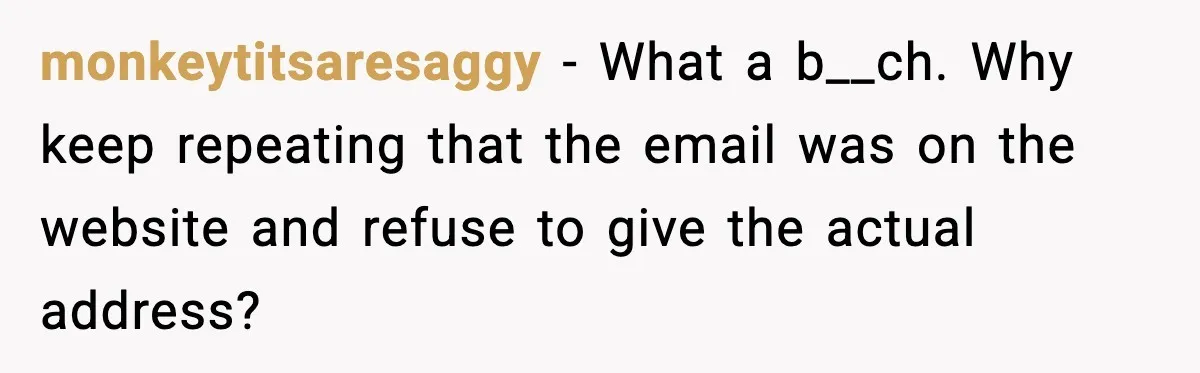

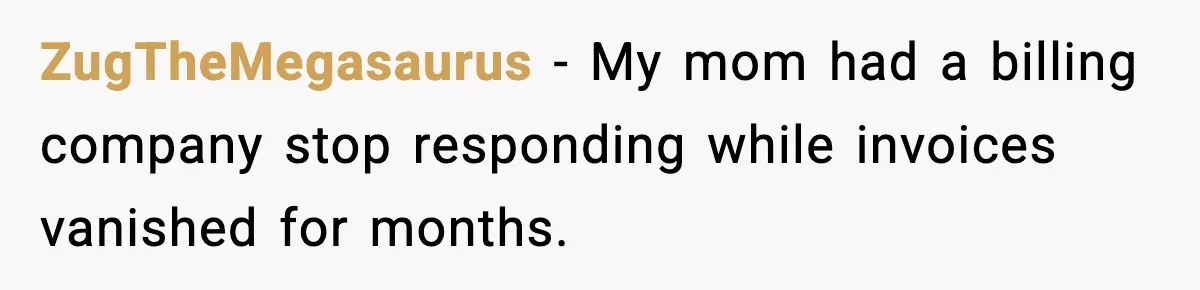
Another group chimed in with “been there, done that, wanted to scream.” These commenters swapped their own stories about giant systems, vanished responses, and the magical power of copying senior people once the front door stops opening.



![Man Emails 300 Hospital Staff After Employee Refuses to Share the Right Address [Reddit User] - Brilliant. Is it Tasmanian? It honestly sounds like our healthcare.](https://dailyhighlight.com/wp-content/uploads/2026/03/wp-editor-1773048839467-5.webp)


A smaller group brought the reality check. One commenter pointed out that privacy rules do matter, even when the staff member handling the call acts wildly unhelpful. Fair enough, because bureaucracy can be both technically correct and deeply maddening at the same time.




What makes this story stick is not only the malicious compliance. It is the chain reaction behind it.
A wife tried to help. A staff member chose the most unhelpful possible version of “help.” A patient who had already waited far too long decided to follow instructions so literally that the whole hospital network suddenly remembered how email works.
There is something funny here, obviously.
The image of one sharply worded message landing in hundreds of inboxes at once has real chaos-goblin energy. But there is also something sad underneath it. People should not need a mini communications blitz to confirm they still exist on a waiting list.
Stories like this usually travel because they tap into a shared fear. Most of us worry that if we stay quiet too long, our paperwork, request, referral, or name will just drift into the void.
That is why advocacy matters so much.
So what do you think? Did this guy cross the line by emailing hundreds of hospital addresses, or did he use the only language bureaucracy was finally willing to hear? And honestly, after that phone call, would you have done anything differently?